
The point of cleaning and sanitizing throughout the hospital is, above all else, creating a pleasant, safe environment for both healthcare professionals and patients. This way, all stakeholders are helping reduce the microbial load present on surfaces and the risk of transmission of health care-associated infections (HCAIs).
Good sanitation is not an isolated activity. First, sanitation must be understood as a set of practices that contribute to the aim of ensuring a clean environment that’s free of potential contaminants. Undesirable materials must be removed from surfaces and floors. This includes organic matter, chemical residues, and microorganisms. Remaining residues must present no threats to the quality and safety of patients or professionals.
Despite this, a series of factors we’re often unable to control means that some places continue to be contaminated or infected in hospitals. These require using other courses of action. According to some studies, proper cleaning and sanitation eliminate between 80 and 85% of microorganisms present. If we apply a disinfectant after cleaning, this percentage can increase to 90-95% of microorganisms.
Bio-decontamination, a key process in sanitation
So what can be done to kill the remaining microbes? In these cases, we can turn to bio-decontamination. This can be done with the right chemical products, which are primarily made with phenols, quaternary ammonium, alcohols, and so on. These solutions can be used in all hospital settings. They offer good results since they act against a wide range of bacteria, fungi, and viruses. They’re easy to use and don’t require spaces to be evacuated for a long period. However, some strains of bacteria are multi-resistant and spread through spores that aren’t eliminated.
There are several methods to address this. In this article, we’ll only look at vaporous bio-decontamination with hydrogen peroxide and ultraviolet radiation (UV-C) bio-decontamination.
With vaporized hydrogen peroxide, the concentration used may vary from 3 to 19%, depending on the level of decontamination needed. This method requires closing off the space that’s being decontaminated; after vaporizing, you must wait about 90 minutes before using the space again. It should be noted that it is a residue-free process. This means that, after the waiting period, the decontaminated areas may be used right away.
This procedure is more effective in controlling and reducing multi-resistant pathogenic microorganisms than conventional sanitation for spaces. It’s quite practical as it doesn’t require taking down curtains and does enable decontaminating f medical and/or electronic equipment. That way, the risk of infections and cross-contamination is reduced. As a result, the quality of services provided to users is higher, and the downtime for treated areas is reduced, thereby increasing the service’s productivity.
Another example currently available is a disinfection solution for hospital facilities using ultraviolet radiation (UV-C), which is emitted by special lamps that can be stationary or mobile, the latter being paired with autonomous robots. UV-C radiation eliminates pathogens like bacteria, fungi, and viruses in a short time – a test carried out by Boston University found that a UV radiation dose of 5mJ/cm² could deactivate 99% of the SARS-CoV-2 virus on surfaces with an exposure time of only 6 seconds. Based on this data, researchers extrapolated that a dose of 22 mJ/ cm² for 25 seconds would allow for a 99.9999% reduction. Signify solutions were used in this study.
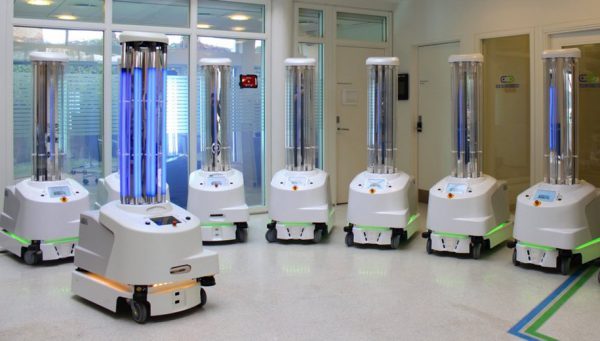
UV-C radiation can break down the DNA and RNA of bacteria, viruses, and spores, rendering them harmless. To date, no known viruses or bacteria have been proven immune to this method.
Risk reduction
The main advantages of using this type of equipment for disinfection are:
- Reducing contamination risks for both healthcare professionals and patients.
- Creating a feeling of protection and safety for the facilities’ users.
- Reducing the use of chemical products and thus being more environmentally friendly.
Using any of these disinfection/bio-decontamination processes is directly proportional to patients’ and professionals’ safety, given the inherent reduction in exposure to potentially infectious agents. Patients being able to observe the best hygiene and cleanliness conditions in hospitals is recognized as a factor in their satisfaction. This translates into a feeling of trust, which often helps in their recovery.
We’re so acutely impacted by this pandemic right now, and the world is seeing an increasingly rapid and frequent spread of diseases. Therefore, it is important for those responsible for these facilities to reflect on the benefits of implementing bio-decontamination routines whose intensity suits their specific location’s particularities and needs.





There are no comments yet